On Tuesday morning, Samuel's ventilator was wheeled out of his room. The machine that has kept him breathing for his 11 weeks of life is gone. I was a bit superstitious about them actually taking it away but it was already gone when I arrived that morning. In two weeks, we have said good-bye to the endo-tracheal tube, the ventilator and the great big oxygen mask.
We also said good-bye to Samuel's PICC line on Tuesday. He was on a month-long course of antibiotics for the infected blood clot he got through his femoral line but he completed those antibiotics on Monday. No more IV infusions for so the last central line came out. We celebrated with Samuel's first ever tub bath. He wasn't all that impressed with this marker of his new line-free status but his nurse Lindsay and I enjoyed it immensely.
And one more good-bye for Tuesday... Samuel managed to loop his tiny baby finger around his NJ tube and yank it out. Of his intestine. Nice work, Sam. CPAP pushes air into the stomach and can cause discomfort and vomiting if there is food there as well. So Samuel has had an NJ into his intestine to by-pass his stomach for feeding and medications, plus an NG into his stomach for venting air.
Getting a new NJ tube in is challenging since Samuel's anatomy is still a bit mixed up. After a couple of tries, they opted to try feeding him with the tube in his stomach to see how he would do - a risky maneuver that has paid off. Samuel is now on full feeds via NG. He has been much more content in the last day or so, which may be in part because he has a full tummy again. Who doesn't like a full tummy?!
The only dark spot on the near horizon is that the big boys and I have all had colds and I am fretting that Samuel will get it too. What is just some stuffy noses and coughing for us could be some enormous steps backwards for Samuel. If he can stay healthy, they will keep weaning his pressures on the oxygen and he could go to the Unit in a week or so. I will miss the beautiful people who I have grown attached to in our time at the ICU but I know the Unit is one step closer to bringing our baby home.
 |
| Trying out the new nasal cannula. The skin breakdown on his nose is from the big mask. The duoderm is still on his chin in case we had to go back to BiPAP. |
 |
| Cuddling is so much easier without the PICC line and the oxygen mask. We are now down to six tubes to manage! |
 |
| Wide awake and cozy in blankets. That little face is healing now. |
 |
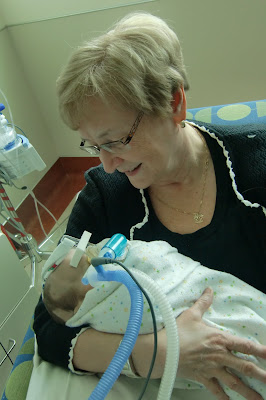
| Asleep in Nana's arms. |